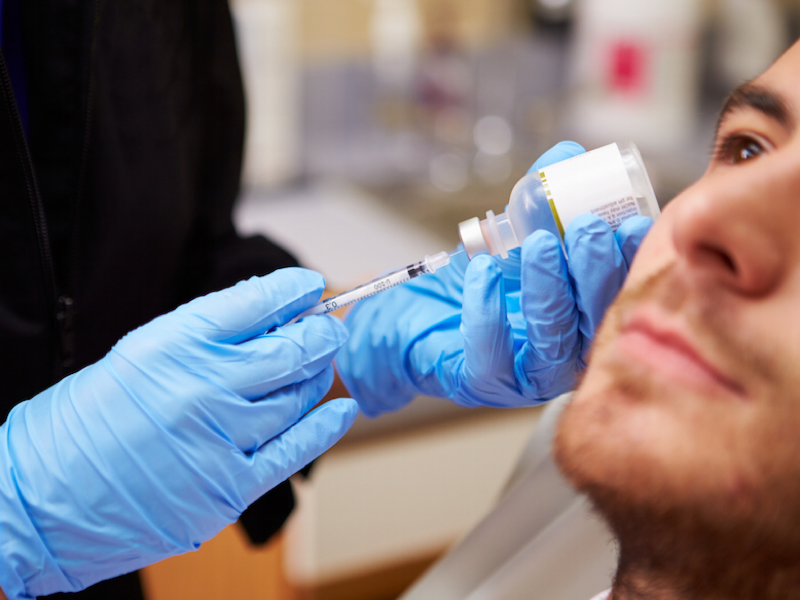
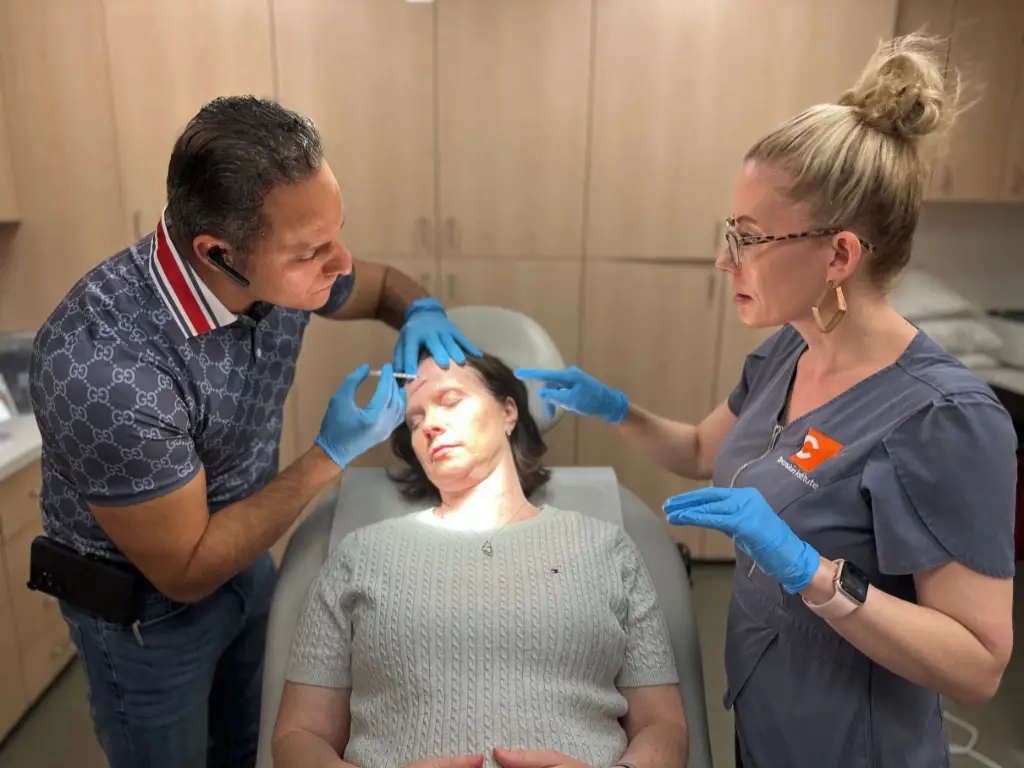
Share with the patient that the best use for Botox® is preventative… NOT reparative.
By starting Botox® every 4 months in your late 20s or early 30s, patients effectively avoid the years of scrunching and frowning which inevitable lead to furrows.
Botox® is, indeed, “a stitch in time”.
Always take your time during the initial consultation to “read the patient.” Realistic expectations as well as what they perceive to be the “problem to be fixed” are so crucial to happy outcomes.
Make it a point to study each face prior to injecting and go through the exercise of having the patient make a series of movements that allowed the physician to see exactly how the muscles interact.
Show patients in the mirror what specifically they can expect to have improved; have patients smile big, note the wrinkles around the eyes both at rest and during a smile.
Then show them what will be different after Botox® injection, i.e. “when one smiles, no wrinkles will bunch up here at said discrete location.”
Always use Before and After photos…they can be your best friend as people forget what they looked like prior to their treatment.
When taking before pictures of each patients, USE available light rather than flash so as not to wipe out the guide marks if made with a white pencil.
Alternatively, use an eyeliner to mark the injection sites. Eyeliner is easy to remove with minimal rubbing.
Furthermore, when marked with white pencil on the affected areas, indicate with a dot for each injection site, and create a facial map for future treatments.
A single Botox® injection of 2-4 units will cover a 2cm diameter area, and placed carefully it can be extremely aesthetic.
Try to find out during the initial consultation if a patient has had Botox® treatments and if so, what things worked and did not work with the previous injections.
Look for things to avoid to replicate; also this is a useful strategy to determine if a patient has unrealistic expectations or body dysmorphic disorder etc.
Ask patients to avoid any medicine that may increase their potential for bruising for at least two weeks prior to injection (i.e. aspirin, ibuprofen, etc.)